Patients with the most aggressive and fatal form of brain tumour, called glioblastoma, are being offered a more detailed diagnosis and tailored treatment plan, based on genomic sequencing results turned around within ten days.
Using cutting-edge genomics technology, the Minderoo Precision Brain Tumour Programme (MPBTP) is establishing the first-ever precision medicine system for brain cancer patients on the NHS, with the potential to revolutionise brain cancer treatment and improve survival rates.
The programme is a partnership between Cambridge University Hospitals NHS Foundation Trust (CUH), Minderoo Foundation, the Tessa Jowell Brain Cancer Mission, NHS East Genomics Laboratory Hub, Cancer Research UK Cambridge Centre at the University of Cambridge and Illumina.
The ambition is to inspire, inform and ultimately improve the standard of care for all patients with brain cancer.
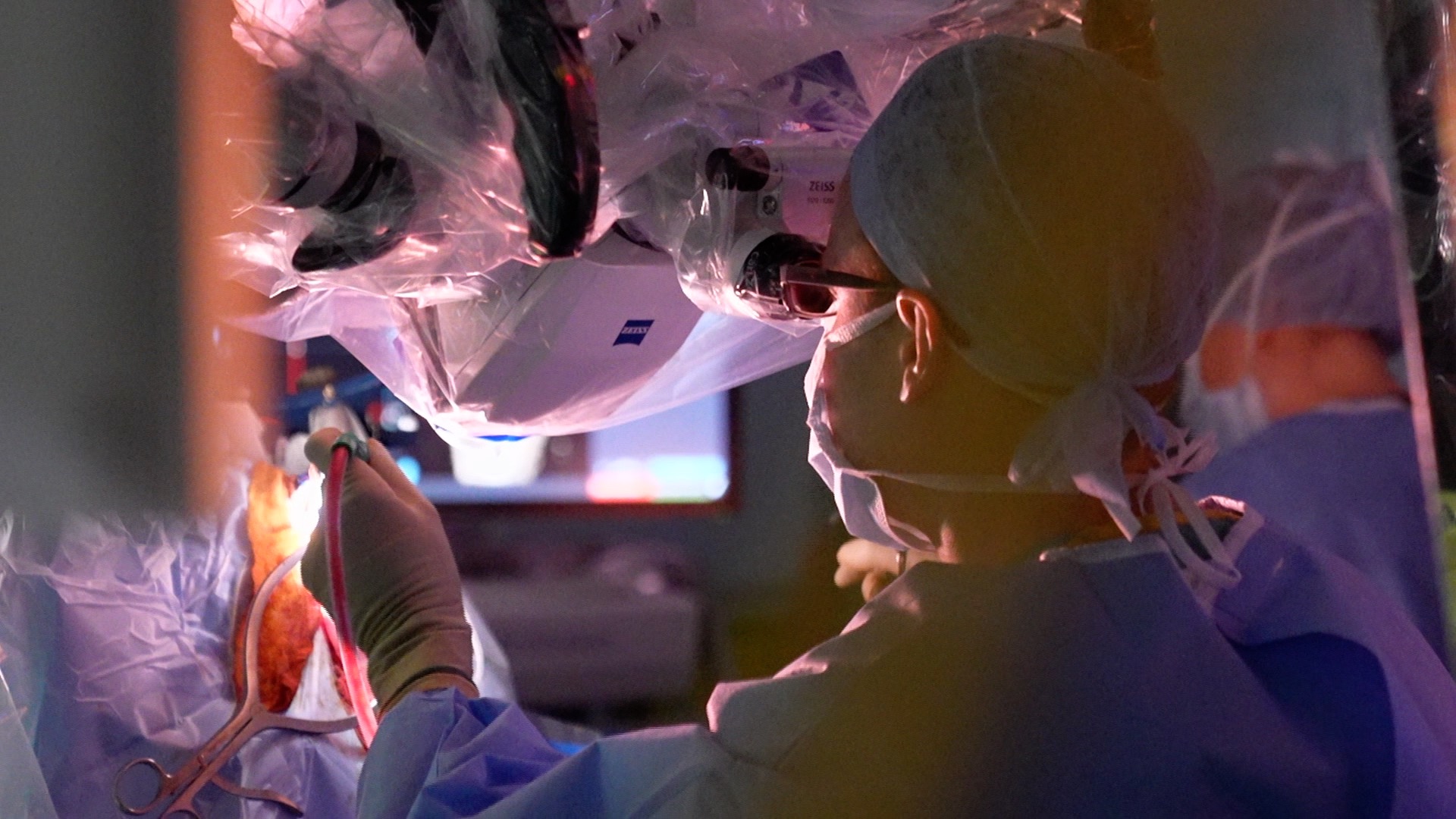
34 year old Daniel Covington is part of the Minderoo Precision Brain Tumour Programme (MPBTP) at Cambridge University Hospitals NHS Trust. He was diagnosed with a brain tumour towards the end of last year and underwent surgery a few weeks later to debulk as much of the tumour as possible.
In ten days, the tumour genome had been sequenced and the results were discussed at a genomics tumour advisory board meeting at Addenbrooke's Hospital to identify the best treatment. This means Daniel was able to access a personalised treatment plan from the time of his initial diagnosis.
Mr Richard Mair, consultant neurosurgeon at CUH who is leading the MBPTP, said:
“This incredibly exciting new programme enables us to analyse the mutations driving a patient’s tumour in real-time. We hope to use this information to identify whether any new, targeted treatments can be offered to these patients.”
The ultimate goal is to roll out this approach nationally, with the help of the Tessa Jowell Centres of Excellence initiative, and by integrating rapid genomic testing for this group of patients into the NHS Genomic Medicine Service.
UK Ambassador for Minderoo Foundation, Jess Mills is closely connected with the MPBTP. Her mother, the late Baroness Tessa Jowell, spent the final months of her life campaigning for better brain cancer treatments that could be made available to everyone via the NHS.
“I am proud to carry on the campaign my Mum started after she was diagnosed with terminal brain cancer,” Jess Mills said.
“Brain tumours are the biggest cancer killer of children and adults under 40 in the UK, and thanks to the support of Minderoo Foundation, my hope is that every patient with a terminal diagnosis will soon be offered precision treatment, so that they get to have the best chance possible of living and living well with their diagnosis.”
Ms Mills is a founding member of the Tessa Jowell Brain Cancer Mission, established to deliver her mother’s legacy. The MPBTP is part of the Mission's national strategy to innovate brain cancer treatment, leading to universal access to excellence for all.
“Mum felt a great responsibility, as a public servant for more than 50 years, that more should be done for patients that were being let down by the current system. So today there is hope that before long, this revolutionary programme will become the new standard of care for brain tumour patients across the UK, and beyond,” she said.
The MPBTP will also enable researchers unprecedented access to detailed genomic data on brain tumour patients to identify potential therapeutic targets, develop new treatments and offer innovative clinical trials.
“The focus on this rare but really aggressive tumour type is critical,” said Prof Richard Gilbertson, Director of the Cancer Research UK Cambridge Centre at the University of Cambridge.
“Because Minderoo has an interest in uniting patient data from across the globe, this helps us work with colleagues around the world effectively, bringing together everything we learn from patients, wherever they live, so we can build a more complete understanding of this terrible disease.”
Minderoo Foundation Co-Chair Nicola Forrest AO said collaboration was at the heart of Minderoo Foundation’s approach and the MPBTP brings together academic, clinical, industry and philanthropic partners to establish the infrastructure and the systems required to develop the first-ever precision medicine system for brain cancer patients in the country.
“Brain cancer research has had little investment over the last several decades so that’s where we decided was most important to focus. At Minderoo Foundation, we seek out the hardest challenges and if we could make a difference there then it could translate across all cancers,” Mrs Forrest said.
Dr David Bentley, Vice President & Chief Scientist, Illumina, said: “We are delighted to embark on this project with the Addenbrooke’s team, and to see how our genomics expertise can best help patients suffering from this debilitating cancer now and in the future.”
Offering precision cancer treatment to patients, such as the MPBTP, is a key aim of the new Cambridge Cancer Research Hospital bringing together clinical expertise from Addenbrooke's with cutting-edge research from the Cancer Research UK Cambridge Centre and University of Cambridge.
The new specialist cancer hospital will combine modern NHS clinical space with three new research institutes dedicated to fulfilling the ambitions set out in the government's Life Science Strategy and the NHS Long Term Plan.
This unique facility will change the story of cancer for patients – in this region, nationally and globally – by detecting cancer earlier, diagnosing it more accurately, and treating it more precisely.
How the Minderoo Precision Brain Tumour Programme works
- When the patient undergoes brain surgery at Addenbrooke's, a tumour sample is taken along with a benchmark blood sample.
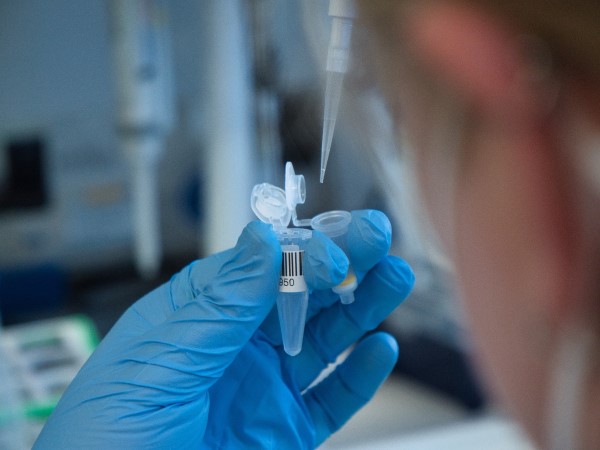
- The samples are sent to the Illumina Centre in Cambridge for complete genomic sequencing (DNA from patient’s blood, which is the patient’s ‘normal’ genomic code, is compared with the DNA and RNA from the tumour sample) to identify specific genomic mutations present in the tumour.
- In just ten days the genomic results are returned to Addenbrooke’s and discussed at a genomics tumour advisory board meeting – including clinicians, researchers and data analysts – to decide on the best course of treatment.
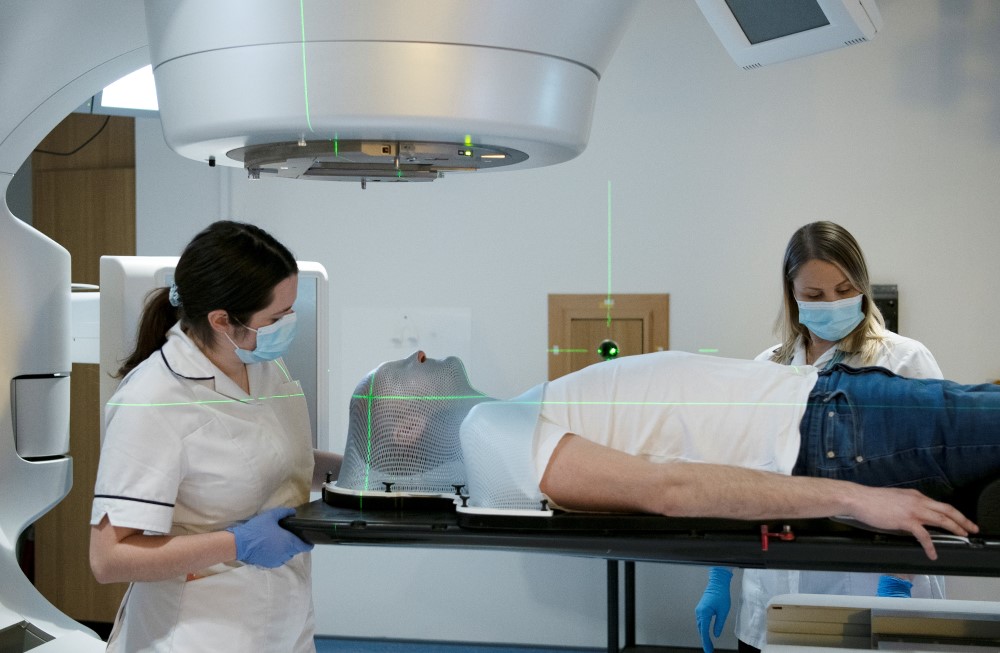
- This means the patient is given a personalised treatment plan based on the type of brain cancer they have as soon as possible, identifying treatments most likely to work and avoiding treatments that may not be effective. Patients will have the extra confidence that the treatment they are receiving is their best option.