An army of cells constantly patrols within us, attacking anything it recognises as foreign, keeping us safe from invading pathogens. But sometimes things go wrong: the soldiers mistake benign cells for invaders, turning their friendly fire on
us and declaring war.
The consequences are diseases like multiple sclerosis (MS), asthma, inflammatory bowel disease, type 1 diabetes and rheumatoid arthritis – diseases that are increasing at an alarming rate in both the developed and developing worlds.
Cambridge will be ramping up the fight against immune-mediated and inflammatory diseases with the opening next year of the Cambridge Institute of Therapeutic Immunology and Infectious Disease, headed by Professor Ken Smith. The Institute will work at the interface between immunity, infection and the microbiome (the microorganisms that live naturally within us). “We’re interested in discovering fundamental mechanisms that can turn the immune system on or off in different contexts, to modify, treat or prevent both inflammatory and infectious diseases,” says Smith.
But while diseases such as Crohn’s and asthma have long been understood to be a consequence of friendly fire, scientists are starting to see this phenomenon give rise to more surprising conditions, particularly in mental health.
In 2009, Professor Belinda Lennox, then at Cambridge and now at Oxford, led a study that showed that 7% of patients with psychoses tested positive for antibodies that attacked a particular receptor in the brain, the NMDA receptor. This blocked a key neurotransmitter, affecting communication between nerve cells and causing the symptoms.
Professor Alasdair Coles from Cambridge’s Department of Clinical Neurosciences is working with Lennox on a trial to identify patients with this particular antibody and reverse its effects. One of their treatments involves harnessing the immune system – weaponising it, one might say – to attack rogue warriors using rituximab, a monoclonal antibody therapy that kills off B-cells, the cells that generate antibodies.
“You can make monoclonal antibodies for experimental purposes against anything you like within a few days,” explains Coles. “In contrast, to come up with a small molecule – the alternative sort of drug – takes a long, long time.”
The first monoclonal antibody to be made into a drug, created here in Cambridge, is called alemtuzumab. It targets both B- and T-cells and has been used in a variety of autoimmune diseases and cancers. Its biggest use is in MS, where it eliminates the rogue T- and B-cells that attack the protective insulation (myelin sheath) around nerve fibres. Licensed in Europe in 2013 and approved by NICE in 2014, it has now been used in tens of thousands of MS patients.
As well as treating diseases caused by the immune system, antibody therapies are now widely used to treat cancer. And, as Professor Gillian Griffiths, Director of the Cambridge Institute for Medical Research, explains, antibody-producing cells are not the only immune cells that can be weaponised.
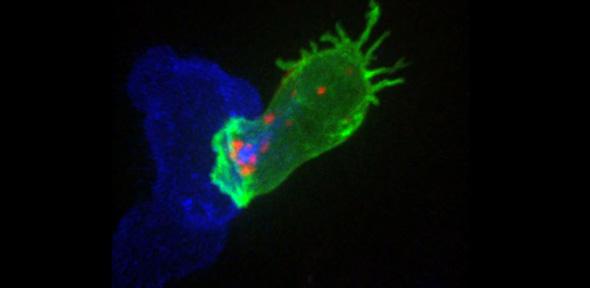
“T-cells are also showing great promise,” she says. “They are the body’s serial killers, patrolling, identifying and destroying infected and cancer cells with remarkable precision and efficiency.”
But cancer cells are able to trick T-cells by sending out a ‘don’t kill’ signal. Antibodies that block these signals, which have become known as ‘checkpoint inhibitors’, are proving remarkably successful in cancer therapies. “My lab focuses on what tells a T-cell to kill, and how you make it a really good killer, using imaging and genetic approaches to understand how these cells can be fine-tuned,” Griffiths explains. “This has revealed some novel mechanisms that play key roles in regulating killing.”
A second, more experimental, approach uses souped-up cells known as chimeric antigen receptor (CAR) T-cells programmed to recognise and attack a patient’s tumour.
Neither approach is perfect: antibody therapies can dampen down the entire immune system, causing secondary problems, while CAR T-cell therapies are prohibitively expensive as each CAR T-cell needs to be programmed to suit an individual. But, says Griffiths, “the results to date from both approaches are really rather remarkable”.
One of the problems that’s dogged immunotherapy trials is that T-cells only have a short lifespan. Most of the T-cells transplanted during immunotherapy are gone within three days, nowhere near long enough to defeat the tumour.
This is where Professor Randall Johnson comes in. He’s been working with a molecule (2-hydroxyglutarate), which he says has “become trendy of late”. It’s an ‘oncometabolite’, believed to be responsible for making cells cancerous, which is why pharmaceutical companies are trying to inhibit its action. Johnson has taken the opposite approach.
He’s shown that a slightly different form of the molecule plays a critical role in T-cell function: it can turn them into renewable cells that hang around for a long time and can reactivate to combat cancer. Increasing the levels of this molecule in T-cells makes them stay around longer and be much better at destroying tumours. “Rather than creating killer T-cells that are active from the start, but burn out very quickly, we’re creating an army of cells that can stay quiet for a long time, but will go into action when necessary.”
This counterintuitive approach caught the attention of Apollo Therapeutics, who recognised the enormous promise and has invested in Johnson’s work, which he carried out in mice, to see if it can be applied to humans.
But T-cells face other problems, particularly in pancreatic cancer, explains Professor Duncan Jodrell from the Cancer Research UK Cambridge Institute, which is why immunotherapy against these tumours has so far failed. The problem with pancreatic cancer is that ‘islands’ of tumour cells sit in a ‘sea’ of other material, known as stroma. As Jodrell and colleagues have shown, it’s possible for T-cells to get into the stroma, but they go no further. “You can rev up your T-cells, but they just can’t get at the tumour cells.” They are running a study that tries to overcome this immune privilege and allow the T-cells to get to the tumour cells and attack them.
Tim Eisen, Professor of Medical Oncology at Cambridge and Head of the Oncology Translational Medicine Unit at AstraZeneca, believes we can expect great advances in cancer treatment from optimising and, in some cases, combining existing checkpoint inhibitor approaches.
Eisen is working with the Medical Research Council to trial checkpoint inhibitor antibody therapies as a complement – ‘adjuvant’ – to surgery for kidney cancer. Once the kidney is removed, the drug is used to destroy stray tumour cells that have remained behind. But even antibody therapies, which are now widely used within the NHS, are not universally effective and can cause serious complications. “One of the most important things for us to focus on now is which immunotherapeutic drug or particular combination of drugs might be effective in destroying tumour cells and be well tolerated by the patient.”
T-cell therapies – and, in particular, CAR T-cell therapies – are “very exciting, futuristic and experimental,” he says, “but they’re going to take some years to come in as standard therapy.”
The problem is how to make them cost-effective. “It’s never going to be easier to engineer an individual person’s T-cells than it is to take a drug off the shelf and give it to them,” he says. “The key is going to be whether you can industrialise production. But I’m very optimistic about our ability to re-engineer processes and make it available for people in general.”
We may soon see an era, then, when our immune systems become an unstoppable force for good.
Our immune systems are meant to keep us healthy, but sometimes they turn their fire on us, with devastating results. Immunotherapies can help defend against this ‘friendly fire’ – and even weaponise it in our defence.

The text in this work is licensed under a Creative Commons Attribution 4.0 International License. For image use please see separate credits above.















